Element 2
DIFFERENT WAYS INFECTIONS ARE SPREAD

Standard precautions are a set of infection control practices used to prevent transmission of diseases that can be acquired by contact with blood, body fluids, non-intact skin (including rashes), and mucous membranes. These measures are to be used when providing care to all individuals, whether or not they appear infectious or symptomatic. Standard precautions involve standards for hand hygiene, personal protective equipment (PPE), disinfecting and cleaning, waste disposal, and respiratory hygiene (cough etiquette).
To access “Infectious Disease – How do we Control them? video – https://www.youtube.com/watch?v=2JWku3Kjpq0
Contact Transmission

1) Direct Contact is transmission of an infectious disease by exposure to a person with the disease. There is direct contact with blood or other body fluids. Examples of direct contact transmission include kissing, hand shaking, sexual intercourse, bathing a patient, and providing any direct care activities. Specific diseases include mycoplasma pneumonia (pneumonia), Hepatitis A and B (blood virus), conjunctivitis (pink eye), Anthrax (lung and skin disease), influenza (flu), measles, herpes simplex (cold sores), and pertussis (whopping cough).

2) Indirect Contact is transmission of an infectious disease by exposure to a contaminated object or surface or vectors, there is non-human to human contact. Examples of indirect contact transmission include medical instruments, telephones, beds, washroom surface, bedside rail, doorknobs, food tray, contaminated instruments, needles, or dressings, or contaminated gloves that are changed between activities.
Employees must utilize Contact Precautions to prevent spread if pathogens from an infected person through direct (touching) or indirect (touching surfaces or objects in the person’s environment) contact.
For Contact Precautions use:
- Gloves for possible contact with an infected person.
- Washing hands thoroughly
- Disinfect surface, equipment, and objects well
Use Contact Precautions for suspected or documented:
COVID-19 (coronavirus), infectious diarrhea in diapered/incontinent persons, Norwalk Virus (stomach flu), Group A strep wound infections, viral conjunctivitis (eye), and lice, scabies (hair and skin insects that cause damage or disease).

How to Reduce the Spread of Illnesses through Direct or Indirect Contact
To reduce the spread of superficial skin infections, follow hand washing and cleanliness guidelines:
- Make sure staff and children wash their hands after contact with any body fluids. Wear disposable gloves when possible.
- Use free-flowing water for hand washing, if possible. Do not use basins or stoppered sinks, which can become contaminated with the germs.
- Use liquid soap dispensers whenever possible.
- Always use disposable tissues or towels for wiping and washing.
- Never use the same tissue or towel for more than one child.
- Dispose of used tissues and paper towels in a lined, covered step can which is kept away from food and materials/equipment.
How to Reduce the Spread of Diseases through Contact with Blood and Other Body Fluids
You should treat all blood and body fluids as if they were contagious. Always wear protective gloves when handling blood or body fluids containing blood. If gloves are not available, maintain a barrier between the blood and one’s hand through the use of thick towels or gauze.
Prevention is critical! Transmission of illnesses spread through blood is very rare in some settings, and illnesses such as Hepatitis, HIV/AIDS are not spread by casual, daily contact with infected persons. However, Hepatitis and HIV can be transmitted where there is blood contact. For example:
- Touching blood while giving first aid with hands or body surfaces that have cuts or open sores
- Collision accidents where the skin of both people is broken and blood is exchanged
- Cleaning up blood after an accident with hands that have cuts or open sores
- Needle sticks from syringes or other sharp objects.
- Medical, health, beauty treatments or procedures where the skin is punctured or broken
- Unclean equipment with blood on it such as razors, scissors, razors, etc.
- The only way blood-to-blood exchange can happen through biting is for the following events to occur:
- There is an injury to the mouth of the biter.
- The bite creates a wound so serious that the skin is broken and blood flows.
- Blood is exchanged.

Droplet Transmission
Droplet transmission is exposure to infectious disease through inhalation of pathogens suspended on liquid particles. Examples of droplet transmissions are coughing and sneezing. Workers must utilize Droplet Precautions to prevent droplet (larger particle) transmission of infectious agents when the patient talks, coughs, or sneezes.
For Droplet Precautions use:
- Elbow to cover nose and mouth when sneezing.
- Wash hands thoroughly
- Disinfect surfaces, objects, and equipment well
Use Droplet Precautions for documented or suspected:
COVID-19 (coronavirus); pneumonia, scarlet fever (lung and skin infections); H. Influenza meningitis, epiglottitis (lung and throat infection); Influenza, Mumps, Rubella (lung infection); Meningococcal infections (brain infection).

How to prevent Droplet Infections:
- Source control:put a mask on the person or wear a mask around person coughing.
- Ensure appropriate patient placement in a single room if possible and instruct person to follow Respiratory Hygiene/Cough Etiquette recommendations (Cover nose/mouth with a tissue coughing or sneezing. When coughing, use a mask. Use disposable tissues and discard after use.)
- Use personal protective equipment (PPE) appropriately.Put on mask going into person’s home or around person. You may need to wear other personal protective equipment depending on what you are doing such as gown or apron, gloves and so forth. (CDC, 2016)

Respiratory hygiene/cough etiquette
Avoid public places when experiences flu symptoms and cover your cough. It is advisable that personnel and visitors areas must have disposable hand washing equipment near sinks, or no touch hand-sanitizers, tissue and non-touch trash receptacles.
Employees should be vigilant when dealing with infectious diseases. Early identification, prompt isolation, and appropriate treatment is essential to prevent the spread to children, personnel and clients.

Control of routes of Droplet Infection Spread
- Hand hygiene. A general term that applies to hand washing, antiseptic hand wash or antiseptic hand rub is one of the best ways to prevent transmission of infectious diseases. [Standard Precautions mandates disinfecting hands immediately after removing gloves.]
- Wearing gloves is crucial when possible exposure is anticipated. Glove selection should be based on the potential for exposure and the task that is being executed. [The use of petroleum based hand lotions or creams (like Vaseline) can impair the integrity of latex gloves, weakening them and increasing their permeability (weaken gloves and allows things to go through gloves).]
- Other significant ways to protect childcare personnel and children is by utilizing vaccination, protecting immune system and maintain a health diet.

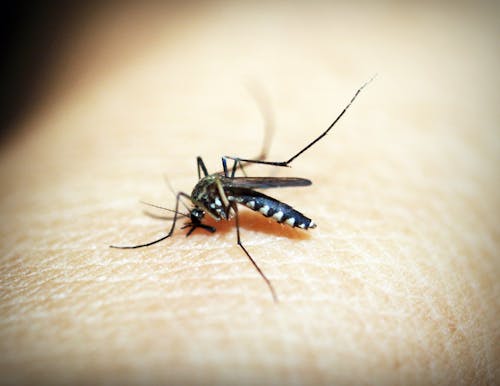
Vector Transmission
Vector transmission is transmission of an infectious disease by a vector. Vectors are animal or insects capable of spreading diseases. Vectors spread diseases through contact with susceptible host, food, and a common touch surface. Examples of vectors include mosquitoes, rats, dogs, flies, mites, and fleas. Vectors spread disease such as malaria, yellow fever, dengue fever, West Nile virus from mosquitoes; Rocky Mountain spotted fever (from ticks), and Lyme disease (from ticks).
Common vehicle of transmission refers to pathogens transmitted to the host by contaminated items such as food, water, medications, devices, and equipment.
** We are still learning about this virus, but it appears that it can spread from people to animals in some situations (CDC, 2020) **

PREVENTION STRATEGIES
- Hand washing – always – following any patient contact. Wash hands for at least 20 seconds with soap and warm water – especially if visibly soiled. Clean hands with alcohol- based hand rub if not visibly soiled.
Virus 
Airborne Borne Precautions
Airborne precautions are required to protect against spread of infectious agents in the air. Diseases requiring airborne precautions include but are not limited to: COVID-19 (coronavirus), Measles, Severe Acute Respiratory Syndrome (SARS) (lung disease), Varicella (chickenpox), and Mycobacterium tuberculosis (TB, tuberculosis).
Preventing airborne spread requires personal respiratory protection and special ventilation and air handling (MNDOH, 2020).

How airborne transmission occurs:
Airborne transmission occurs through the spreading of either:
- airborne droplet nuclei (small-particles [small particle] of droplets containing germs that remain suspended in the air for long periods of time) or
- dust particles that contains the germ
Microorganisms carried by the airborne route can be widely spread by air currents and may become inhaled by a person in the same room or over a long distance from the source person – depending on environmental factors such as temperature and ventilation (fresh air) (MNDOH, 2020).

How to Reduce the Spread of Airborne Illnesses
- Source control: put a mask on the patient.
- Ensure appropriate patient placement in an airborne infection isolation room (AIIR) constructed according to the Guideline for Isolation Precautions. In settings where Airborne Precautions cannot be implemented due to limited engineering resources, masking the patient and placing the patient in a private room with the door closed will reduce the likelihood of airborne transmission until the patient is either transferred to a facility with an AIIR or returned home.
- Restrict susceptible healthcare personnel from entering the room of patients known or suspected to have measles, chickenpox, disseminated zoster, or smallpox if other immune healthcare personnel are available.
- Use personal protective equipment (PPE) appropriately, including a fit-tested NIOSH-approved N95 or higher level respirator for healthcare personnel.
- Limit transport and movement of patients outside of the room to medically-necessary purposes. If transport or movement outside an AIIR is necessary, instruct patients to wear a surgical mask, if possible, and observe Respiratory Hygiene/Cough Etiquette. Healthcare personnel transporting patients who are on Airborne Precautions do not need to wear a mask or respirator during transport if the patient is wearing a mask and infectious skin lesions are covered.
- Immunize susceptible persons as soon as possible following unprotected contact with vaccine-preventable infections (e.g., measles (viral lung and kin infection, varicella [chickenpox] or smallpox (viral lung and skin infection). (CDC, 2016).

How to Reduce the Spread of Infections through Stools
Since staff who have digestive illnesses don’t always feel sick or have diarrhea, the best method for preventing the spread of these diseases is to have a constant prevention program (universal precautions) in place at your program. The hepatitis A virus, rotavirus, and giardia lamblia cysts can all survive on surfaces for periods ranging from hours to weeks.
Practice the following:
- Strict enforcement of all hand washing for adults.
- Environmental sanitation with focus on diapering, toileting and food preparation areas.
- Exclusion guidelines: Excluded staff may come back after treatment and when the consistency of diarrhea improves, or with approval of the person’s health provider.
