Lesson 2: COVID-19 (Coronavirus)
What is Coronavirus?
Coronaviruses are a large family of viruses which may cause illness in animals or humans. In humans, several coronaviruses are known to cause respiratory infections ranging from the common cold to more severe diseases such as Middle East Respiratory Syndrome (MERS) and Severe Acute Respiratory Syndrome (SARS). The most recently discovered coronavirus causes coronavirus disease COVID-19. (WHO, 2020).
SARS-CoV
According to CDC in 2005, “The primary way that SARS appears to spread is by close person-to-person contact. SARS-CoV is thought to be transmitted most readily by respiratory droplets (droplet spread) produced when an infected person coughs or sneezes. Droplet spread can happen when droplets from the cough or sneeze of an infected person are propelled ….through the air and deposited on the mucous membranes of the mouth, nose, or eyes of persons who are nearby. The virus also can spread when a person touches a surface or object contaminated with infectious droplets and then touches his or her mouth, nose, or eye(s). In addition, it is possible that SARS-CoV might be spread more broadly through the air (airborne spread) or by other ways that are not now known.” Therefore, SARS-CoV2 or COVID-19 is likely transmitted via air along with other ways including poop. SARS-CoV mutates or adapts and changes (CDC, 2005, 2020). The 2003 virus is SARS-CoV1, COVID-19 is SARS-CoV2.
What is COVID-19?
COVID-19 is the infectious disease caused by the most recently discovered coronavirus. This new virus and disease were unknown before the outbreak began in Wuhan, China in December 2019. COVID-19 is now a pandemic affecting many countries globally. (WHO, 2020)
COVID-19 is spread by air, on surfaces, and through respiratory droplets expelled by someone who is coughing or has other symptoms such as fever or tiredness. Many people with COVID-19 experience only mild symptoms. This is particularly true in the early stages of the disease. It is possible to catch COVID-19 from someone who has just a mild cough and does not feel ill. (WHO, 2020)
Some reports have indicated that people with no symptoms can transmit the virus. It is not yet known how often it happens. World Health Organization (WHO) is assessing ongoing research on the topic and will continue to share updated findings. (WHO, 2020)
At-Risk Populations
In any population, there are certain individuals who may have a higher risk of complications if exposed to specific diseases. Consumers and employees with anemia or immunodeficiencies (low resistance, easily catch stuff), and those who are pregnant are all considered “high risk.” Also, those who have chronic disease (such as hypertension, diabetes, asthma, anemia), diets lacking important nutrients, or severely ill should also be informed of the possible risks of acquiring an infection. Whenever there is increased risk of exposure to an infectious disease, consult with your licensed health care provider. The licensed health care provider will assess the risk and make appropriate recommendations for treatment or activities.
Older adults and people of any age who have serious underlying medical conditions might be at higher risk for severe illness from COVID-19.
Based on what we know now, those at high-risk for severe illness from COVID-19 are:
- People 65 years and older
- People who live in a nursing home or long-term care facility
People of all ages with underlying medical conditions, particularly if not well controlled including:
- People with chronic lung disease or moderate to severe asthma
- People who have serious heart conditions
- People who are immunocompromised (low resistance, easily catch stuff)
- Many conditions can cause a person to be immunocompromised, including cancer treatment, smoking, bone marrow or organ transplantation, immune deficiencies, poorly controlled HIV or AIDS, and prolonged use of corticosteroids (steroids) and other immune (resistance) weakening medications
- People with severe overweight
- People with diabetes
- People with chronic kidney disease undergoing dialysis
- People with liver disease
- People suffering from alcoholism (CDC, 2020; National Jewish Health, 2020)
Signs and Symptoms of COVID-19
People with COVID-19 have had a wide range of symptoms reported – ranging from mild symptoms to severe illness. (CDC, 2020; National Jewish Health, 2020; WHO, 2020). Symptoms may appear 2-14 days after exposure to the virus. People with these symptoms may have COVID-19:
-
- Dry Cough or cough with mucus
- Tiredness
- Nasal congestion (stuffy nose)
- Conjunctivitis (pink eye)
- Shortness of breath or difficulty breathing
- Fever
- Sweats
- Chills
- Muscle aches and pain
- Sore throat
- New loss of taste or smell
- Headache
- Diarrhea (loose or watery stool)
- Loss of appetite
- Chest pain (especially under the breastbone) and arrhythmia
- Rapid breathing (fast breathing)
- Abnormal blood clotting (blood clots)
- Discoloration (change in color) of fingers or toes (COVID toes) – itching, irritated, red, blue, discolored or painful toes
- Skin rash (skin bumps)
- Bluish lip and skin (Dr. Ester Freeman Massachusetts General Hospital cited by Lee, 2020)
- Dizziness, headache, confusion or delirium, seizure, and impaired balance or coordination (Dr. Ester Freeman Massachusetts General Hospital cited by Lee, 2020)
- Lesions on the hands or feet that resembled frostbite (Dr. Ester Freeman Massachusetts General Hospital cited by Lee, 2020)
- Hair loss (Novant Health, 2020)
- Erectile dysfunction (emedicinehealth, 2020)
When to Seek Emergency Medical Attention
Look for emergency warning signs** for COVID-19. If someone is showing any of these signs, seek emergency medical care immediately
- Trouble breathing
- Persistent pain or pressure in the chest
- New confusion
- Inability to wake or stay awake
- Bluish lips or face (CDC, 2020)
Call your health care provider if you are not sure about your symptoms.
**This list is not all possible symptoms. Please call your medical provider for any other symptoms that are severe or concerning to you. Call 911 or call ahead to your local emergency facility: Notify the operator that you are seeking care for someone who has or may have COVID-19.**
COVID-19 Symptoms
COVID-19 Pneumonia & Acute Respiratory Distress Syndrome
Acute respiratory distress syndrome (ARDS) is life threatening. It is an injury to the lungs caused by infection or trauma. ARDS causes fluid to leak into the lungs. This makes it extremely difficult to breathe and causes a significant lack of oxygen getting into the bloodstream. The lack of oxygen harms the brain, organs and body tissues.
Most people who develop ARDS are already inpatients in the hospital. Treatment includes oxygen therapy to ensure the blood and body have enough oxygen to function properly. Sedation is often used to prevent agitation and shortness of breath. Fluids are managed to prevent build up in the lungs. Pulmonary rehabilitation is used to help ARDS patients recover strength. (National Jewish Health, 2020).
Fever
A fever is technically defined as a body temperature of 100.4° F or higher, according to the Centers for Disease Control and Prevention. This is true for both babies and adults. And a fever isn’t necessarily a bad thing. It is a sign that your immune system is doing its job, fighting off an invader, like a virus or bacteria, in an attempt to prevent it from overtaking your body.
But a fever can be concerning. Aside from how miserable it may make you feel—with sweating, chills, headaches, and fatigue—it could indicate that a serious illness is developing. And an uncontrolled fever could cause seizures or brain damage. So it’s important to pay attention to fevers and respond appropriately. (Peachman, 2020). Fever, chills, sore throat, sweats, cough, and muscle aches are usual signs of viral infections.
**Among children and teenagers aspirin should not be given/taken for viral illnesses because of the possible association with Reye Syndrome. Reye Syndrome is a rare condition that causes confusion, swelling in the brain, and liver damage. Early symptoms of Reye Syndrome include diarrhea, rapid breathing, vomiting, and severe tiredness. Symptoms such as confusion, seizures, and loss of consciousness need emergency treatment.**
Skin
Early reports from Italy and Thailand, stated that some skin doctors report 20% of COVID-19 patients develop skin symptoms such as patchy red rash, broken blood vessels like in dengue fever.
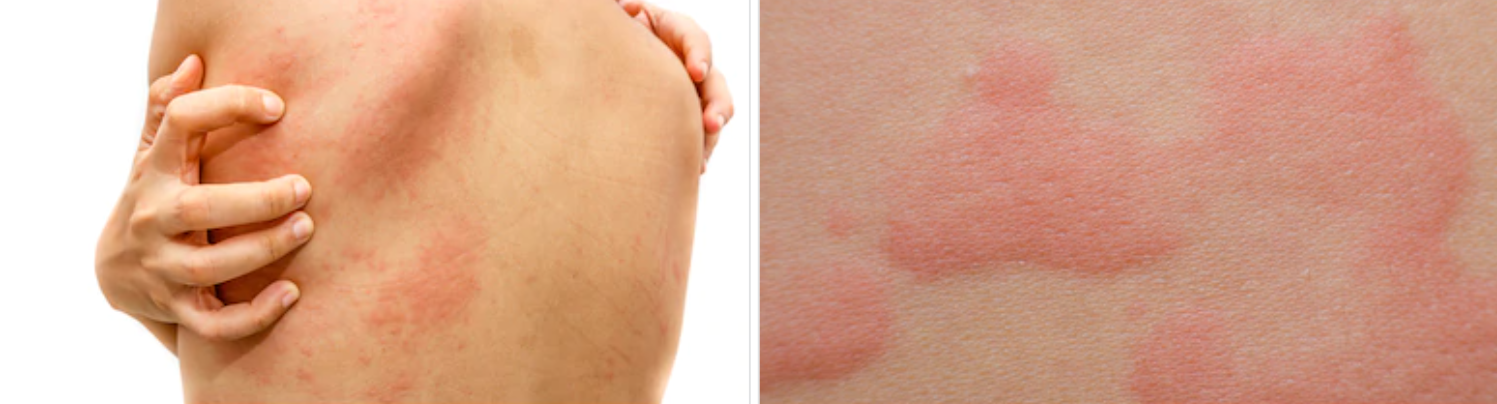
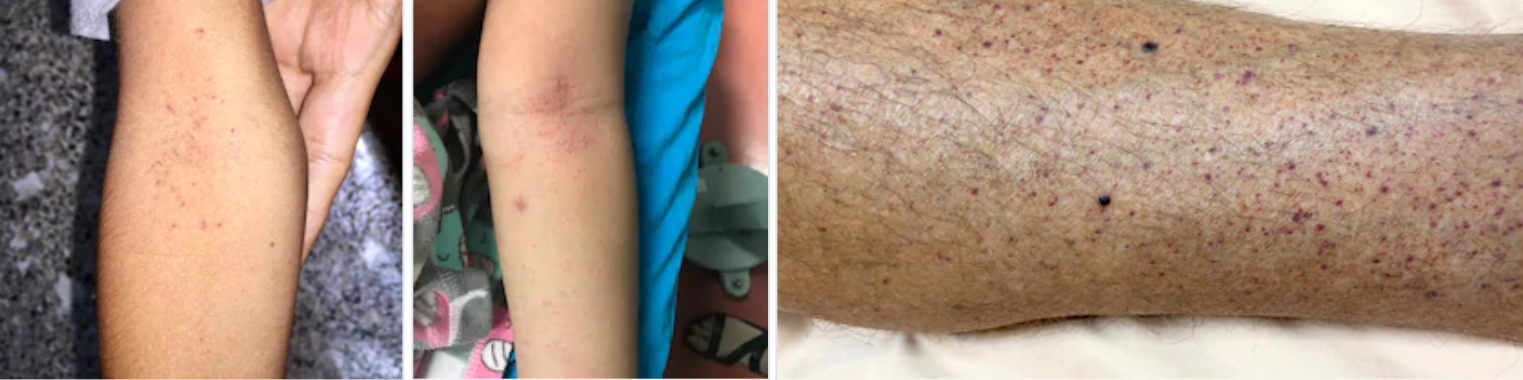
A few developed hives, and one developed chickenpox-like blisters.
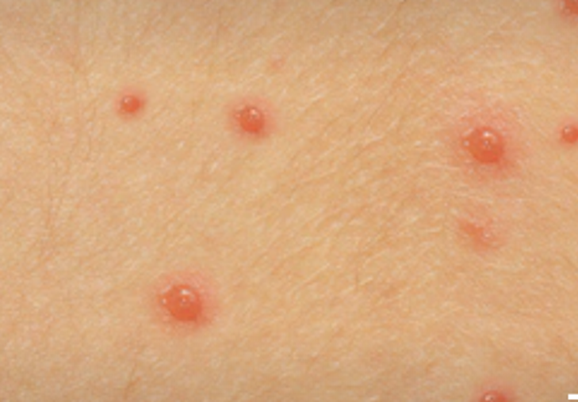
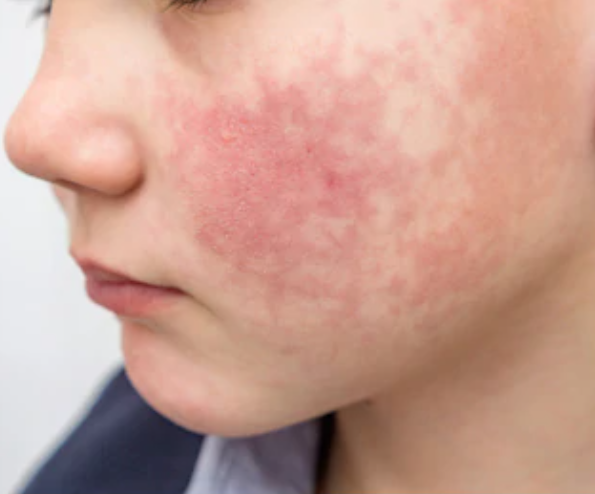
The trunk was the most commonly involved site. Some patients had mottling or blotchy, red marbling of the skin.
There are also reports of toe discolorations red to purple toes known as COVID toes.
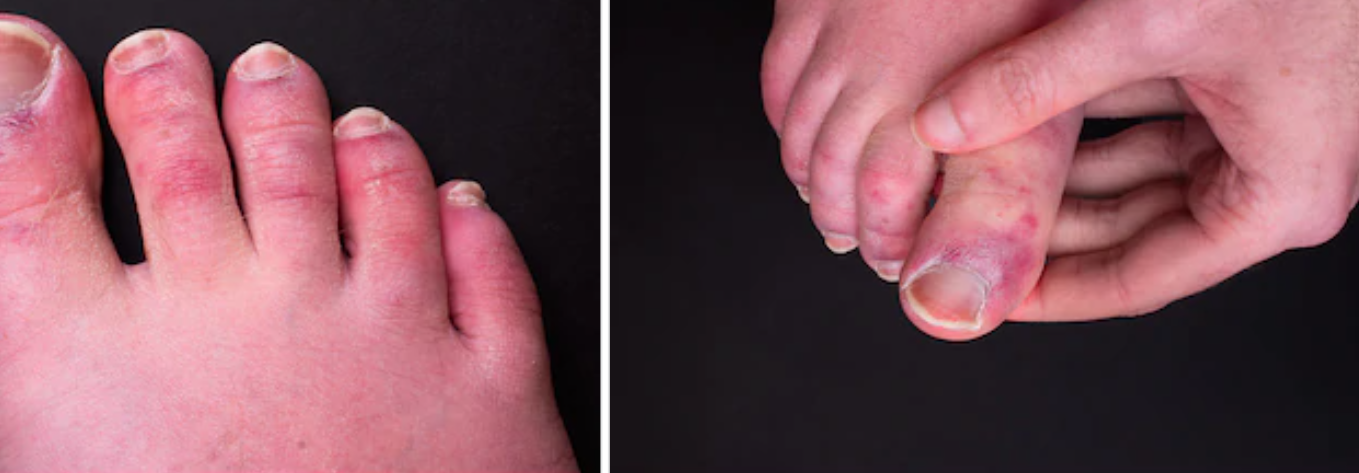
Itchiness of the rash is not a signal of infectiousness or non-infectiousness, however, itching should also be evaluated. A rash can be a symptom of a serious or non-serious condition. Rashes can have an infectious or a non-infectious cause. Deciding what type of rash illnesses can be very difficult and even a licensed health care provider (HCP) will often require lab tests to confirm whether a certain disease is present. (Cleveland Clinic, 2020).
Lungs
Coronavirus can affect the upper respiratory system (nose, sinuses and throat) with flu-like symptoms. In upper lungs, common symptoms of respiratory infections in the nose, sinuses and throat include nasal congestion, runny nose, sore throat, sneezing, achy muscles and headache. Coronavirus upper respiratory infection symptoms also may include cough, diarrhea, fever, shortness of breath and tiredness.
Coronavirus can affect the lower respiratory system (airways and lungs) by causing cough with or without mucous and difficulty breathing. In lower lungs, common symptoms of COVID-19 in respiratory infections in the airways and lungs may include severe cough that produces mucous, shortness of breath, chest tightness and wheezing when you exhale. (National Jewish Health, 2020).
If COVID-19 goes deep into the lungs, it can cause pneumonia. Pneumonia is a concern for older people because they have reduced lung capacity, require longer recover time and have age-weakened immune systems. Pneumonia that is caused by coronavirus may be more severe, affect many parts of the lungs, and cause shock, organ damage, abnormal blood clotting, acute respiratory distress syndrome and deteriorating health. When COVID-19 is severe, it can cause acute respiratory distress syndrome (ARDS) or severe breathing issues.
Sore Throat
A sore throat can be a minor problem, but it can also indicate more significant infections or other serious generalized illnesses. If the sore throat is accompanied by fever, difficulty swallowing, and/or swollen lymph nodes (glands), stay at home, and if needed, notify medical professional and seek medical evaluation.
Cough
Some chronic conditions or allergic conditions are accompanied by a cough. However, a cough may also indicate an infectious disease. Persistent coughs, especially with other symptoms such as episodes of coughing followed by gagging, vomiting, fever, loss of appetite, or weight loss, need medical evaluation. If breathing is labored (breathing hard or difficult), immediate medical referral is indicated.
If there are noticeable lung issues, invest in a pulse oximeter (a device that monitors oxygen levels by placing it on a finger). Typically, normal adult oxygen levels are between 95% and 100%. Any oxygen levels lower than this, contact your medical provider. If lower oxygen level is accompanied skin-color changes, chest pain, increased tiredness, or difficulty breathing, call 911.
Change in Bowel Habit
Diarrhea may accompany a number of infectious diseases. Cramps can be due to inactivity, a change in the ill person’s level of activity, or to dehydration that often occurs during infections. Diarrhea or even apparently normal feces following the resolution of diarrhea may carry an infectious organism that can transmit to others. Some infected individuals may have vomiting or diarrhea, contact health care provider for guidance.
Pain (Head, Back, Limbs, Neck, Stomach)
Muscle aches and pains, headache can also be seen during the course of infectious diseases. Gastrointestinal disturbances such as vomiting, diarrhea, and constipation may be accompanied by abdominal pain.
COVID-19 Complications can include:
- Pneumonia and trouble breathing
- Organ failure in several organs
- Heart problems
- Blood clots
- Acute kidney injury
- Additional viral and bacterial infections (Mayo Clinic, 2020b)
Measures to Promote Good Hygiene in the Workplace
To reduce the risk of infectious diseases in work settings, workplaces should meet certain criteria that promote good hygiene. For example:
- Are there sinks for handwashing as needed?
- Are there separate sinks for preparing food and washing hands? Is food handled in areas separate from the toilets?
- Are the toilets and sinks clean and readily available to staff?
- Are disposable paper towels used?
- Are all doors and cabinet handles cleaned and disinfected at the end of every day?
- Are staff fully immunized (taken vaccines or shots), especially against the flu?
- Is food prepared on site properly handled?
- Is staff instructed to wash their hands throughout the day, including:
- When they arrive for work
- Before and after handling food, or eating
- After using the toilet
- After wiping nose or mouth or tending to a cut or sore
- After handling wastebaskets or garbage
- After handling a pet or other animal
Perform a quick health assessment on yourself each day. It also identifies problems early and reduce the spread of infection.
Signs to Observe
When conducting a health check, you should watch for the following:
- General mood and changes in behavior (sluggish, sleepy)
- Fever or elevated body temperature (sweating or chills)
- Skin rashes, itchy skin, unusual spots, swelling or bruises
- Complaints of pain and not feeling well
- Other signs and symptoms of disease (such as severe coughing, sneezing, breathing difficulties, discharge (stud running) from nose, or eyes, diarrhea, vomiting and so on)
- Don’t go to work. Stay home until you feel better and if necessary, consult with a medical professional if you don’t feel well.
Use All Your Senses to Check for Signs of Illness
- Listen to your body and how you are feeling.
- Is your voice hoarse? Are you having trouble breathing, or coughing?
- Does your skin look pale, have a rash or sores, a runny nose or eyes?
- Feel your cheek and neck for warmth or clamminess (sweaty).
- Do you feel like throwing up or vomited? Or have decreased appetite?
- Have you had more frequent and loose bowel movement?
Using Findings to Make Decisions
If you have concerns about how you look or feel, discuss these problems with your doctor.
Good Hygiene Practices at Work
Personal steps:
- Use proper hand washing.
- Wash hands frequently.
- Use proper cleaning and disinfecting methods.
- Cover open wounds.
- Stay home if you are ill.
- Get seasonal flu vaccine.
- Cover their mouth and nose with a tissue when coughing or sneezing or cough or sneeze into your elbow rather than hands when without a tissue. Put used tissues in a waste basket.
- Avoid touching their eyes, nose, and mouth with their hands.
- Cover open wounds and skin trauma such as abrasions or cuts with a clean dry bandage until healed.
Provide time needed for all staff to wash hands frequently. To remove germs from hands, 20 seconds of rubbing with warm water and soap is required. Alcohol-based hand sanitizers (at least 70% isopropanol alcohol) and wipes are acceptable if soap and water is not available, but washing with soap and water is best.
**[To cleaning your hands with an alcohol-based gel, you rub them together until all of the gel has evaporated and your hands are dry – allowing your hands to dry. Drying provides the full antiseptic effect.]**
When hand washing is necessary:
- When you arrive for work
- After using the bathroom
- Before preparing food or eating
- After touching an infected wound
- After sneezing into hands
When hand sanitizer and hand wipes are acceptable:
- After blowing nose.
- Coughing into hands as long as there is no visible nasal discharge or saliva.
- Touching something that might be contaminated, a keyboard, door knob, railing, etc.
Alcohol-based hand sanitizers should be at least 70% isopropanol alcohol to be effective.
After work:
- Remove shoes and place in a bag by door
- Wash hands immediately
- Place jacket in an area away from other clothes
- Wash face and take a shower as soon as able. Put worn clothes in laundry bag
**Wash clothes in hot water and add a small amount of laundry disinfectant, if available.**
Face Coverings and Social Distancing
People who do not show symptoms may still be able to spread COVID-19. A face covering can help prevent you from spreading COVID-19 to other people. An order from the Governor requires everyone to wear a face covering when outside their home and when they cannot practice physical distancing, such as maintaining 6 feet of distance from others. (NYC Health, 2020b).
Physical Distancing Rules
Orders from the Governor require every New Yorker to stay at home from work, unless they are an essential worker. All non-essential businesses that are normally open to the public must remain closed. Bars and restaurants may provide takeout. All non-essential gatherings of any size for any reason are banned. The police may issue fines to anyone they see in public not following these rules. (NYC Health, 2020b).
COVID-19 Research Updates
It is possible to contract COVID-19 through your eyes. On March 31, 2020 in the Journal of American Medical Association (JAMA) Opthalmology, reported that a study in Hubei Province China found that almost one third of the COVID-19 patients had eyes symptoms and some tested positive for COVID-19 in their eyes (Wu et al., 2020). Another study published June 2, 2020 in the Lancet, found that face mask use reduced risk of COVID-19 infections and N95 or similar masks were better than surgical or similar masks; and eye protection was associated with less infection. According to this study face masks, respirators, and eye protection are best practices for public and health-care settings (Chu et al., 2020).
“If you have goggles or an eye shield, you should use it,” the nation’s top infectious disease expert told ABC News Chief Medical Correspondent Dr. Jennifer Ashton during an Instagram Live conversation on ABC News. When asked if we’re going to get to a point where eye protection is recommended, the director of the National Institute of Allergy and Infectious Diseases responded, “It might, if you really want perfect protection of the mucosal surfaces…You have mucosa in the nose, mucosa in the mouth, but you also have mucosa in the eye,” Fauci continued. “Theoretically, you should protect all the mucosal surfaces. So, if you have goggles or an eye shield you should use it.” (Andreano, 2020).
COVID-19 virus genetic material on surfaces and in the air about 4 meters (13 feet) from patients in two hospital wards in Wuhan, China, posing a risk to healthcare workers. (Van Beusekom, 2020 – University of Minnesota). SARS-CoV-2 was detected in the air as much as 13 feet from the patients – more than twice the 6 feet distance the Centers for Disease Control and Prevention recommends for adequate physical distancing. Further, medical staff tracked the virus on the floor, as indicated by a 100% positive rate in a pharmacy where no patients were allowed (National Safety Council, 2020). It is predicted that peak exhalation speeds can reach up to 33 to 100 feet per second, creating a cloud that can span approximately 23 to 27 feet (7-8 m) (Bourouiba, 2020 – MIT).
“A runner who doesn’t yet know he’s sick running in front of you is likely to infect you with the slipstream behind him by around 30 feet,” Poland said. “At six feet, the largest respiratory droplets have settled out onto the ground.” ““Unless you’re wearing a PAPR, a self-enclosed breathing unit, there’s no such thing as safe,” Poland said. “They’re so-called space suits. The only thing you can be is safer. You can’t be 100% safe with social distancing and face masks.” Gregory Poland, who studies the immunogenetics of vaccine response in adults and children at the Mayo Clinic. (Fottrell, 2020).
COVID-19 Health Evaluation
Whether you are experiencing symptoms that concern you or have questions about rescheduling a procedure that was cancelled, do not hesitate to contact your care provider. They will help you determine next steps that are right for you, and — in many cases — you won’t even have to leave home. (University of Michigan, 2020).
Emergency Care
If you are experiencing life-threatening symptoms, dial 911 or go to your nearest emergency department. Do not delay in seeking emergency care. Waiting too long to seek care for some health care emergencies is a bigger risk to your health than the risk of contracting COVID-19 (University of Michigan, 2020).
Medical Care and Consultation from Home
Some doctors and hospitals offer a number of convenient ways to receive care without leaving your home:
- E-Visits: Patients are instructed to fill out a questionnaire regarding your symptoms for a variety of specific conditions and they receive a quick reply from a provider through the patient portal or emails. If appropriate, diagnostic testing, medications and follow up care can be arranged as part of an E-Visit.
- Video Visits: Experience a live face-to-face visit with a healthcare provider using your smartphone or tablet and some hospitals and clinics have mobile app.
- After-hours primary care phone service: Some health care groups of our primary care clinics offer after-hours phone service staffed by health care providers and/or registered nurses. Some healthcare groups and doctors offer this service is available 365 days a year for established primary care patients.
Also,
- Visit NYC Well’s website, which offers a number of well-being and emotional support applications that can help you cope. If your symptoms of stress become overwhelming, contact NYC Well to speak with a trained counselor 24/7 in over 200 languages (NYC Health, 2020).
- Call the New York State’s COVID-19 Emotional Support Helpline at 844-863-9314 to talk to specially trained volunteer professionals. They will be there to listen, support and offer referrals from 8 a.m. to 10 p.m., seven days a week (NYC Health, 2020).
PRIORITIES FOR COVID-19 (Nucleic Acid or Antigen) TESTING
High Priority
- Hospitalized patients with symptoms
- Healthcare facility workers, workers in congregate living settings, and first responders with symptoms
- Residents in long-term care facilities or other congregate living settings, including prisons and shelters, with symptoms
Priority
- Persons with symptoms of potential COVID-19 infection including: fever, cough, shortness of breath, chills, muscle pain, new loss of taste or smell, vomiting or diarrhea, and/or sore throat.
- Persons without symptoms who are prioritized by health departments or clinicians, for any reason, including but not limited to: public health monitoring, sentinel surveillance, or screening of other asymptomatic individuals according to state and local plans (CDC, 2020).
SARS-CoV-2 can cause asymptomatic (no signs of illness), pre-symptomatic (before signs of illness), and minimally symptomatic infections (few signs of illness), leading to viral shedding that may result in the spread to others who are particularly vulnerable to severe disease and death. Even mild signs and symptoms (e.g., sore throat) of COVID-19 should be evaluated among potentially exposed healthcare personnel, due to their extensive and close contact with vulnerable patients in healthcare settings (CDC, 2020).
How to Discontinue Home Isolation
People with COVID-19 who have stayed home (home isolated) can leave home under the following conditions**
If you have not had a test to determine if you are still contagious, you can leave home after these three things have happened:
-
- You have had no fever for at least 72 hours (that is three full days of no fever without the use of medicine that reduces fevers)
AND - other symptoms have improved (for example, when your cough or shortness of breath have improved)
AND - at least 10 days have passed since your symptoms first appeared
- You have had no fever for at least 72 hours (that is three full days of no fever without the use of medicine that reduces fevers)
If you have had a test to determine if you are still contagious, you can leave home after these three things have happened:
-
- You no longer have a fever (without the use of medicine that reduces fevers)
AND - other symptoms have improved (for example, when your cough or shortness of breath have improved)
AND - you received two negative tests in a row, at least 24 hours apart. Your doctor will follow CDC guidelines. (CDC, 2020)
- You no longer have a fever (without the use of medicine that reduces fevers)
People who DID NOT have COVID-19 symptoms, but tested positive and have stayed home (home isolated) can leave home under the following conditions**:
- If you have not had a test to determine if you are still contagious, you can leave home after these two things have happened:
- At least 10 days have passed since the date of your first positive test
AND - you continue to have no symptoms (no cough or shortness of breath) since the test.
- At least 10 days have passed since the date of your first positive test
- If you have had a test to determine if you are still contagious, you can leave home after:
- You received two negative tests in a row, at least 24 hours apart. Your doctor will follow CDC guidelines. (CDC, 2020)
Note: if you develop symptoms, follow guidance above for people with COVID19 symptoms.
**In all cases, follow the guidance of your doctor and local health department. The decision to stop home isolation should be made in consultation with your healthcare provider and state and local health departments. Some people, for example those with conditions that weaken their immune system, might continue to shed virus even after they recover.** (CDC, 2020)
IMPORTANT UPDATE from CDC
Close Contact – “Someone who was within 6 feet of an infected person for a cumulative total of 15 minutes or more over a 24-hour period* starting from 2 days before illness onset (or, for asymptomatic patients, 2 days prior to test specimen collection) until the time the patient is isolated.” (CDC, October 21, 2020). This means if you were 6 feet or less around someone with COVID-19 but showing no symptoms for 15 minutes, you were in close contact, you could be exposed. Your risk is higher the longer you are around the person. Especially, if the infected person was singing, shouting, coughing in a small space without good air circulation.
CDC. (Oct. 21, 2020). Appendices. Retrieved from https://www.cdc.gov/coronavirus/2019-ncov/php/contact-tracing/contact-tracing-plan/appendix.html#contact
eMedincehealth. (2020). Is Erectile Dysfunction on The Rise During COVID-19 Lockdown? Retrieved from https://www.emedicinehealth.com/erectile_dysfunction_during_covid-19/article_em.htm
Novant Health. (2020). COVID-19 and hair loss – why it’s happening. Retrieved from https://www.novanthealth.org/healthy-headlines/covid-19-and-hair-loss-why-its-happening